PMS are the three letters that all women are familiar with. Women who suffer from PMS experience adverse physical, psychological, and behavioral symptoms during the luteal phase of the menstrual cycle.
But wait – what exactly is the luteal phase?
The luteal phase begins after ovulation, lasts about fourteen days, and ends just before your menstrual period. During this phase, the ruptured follicle closes after releasing the egg and forms the corpus luteum. The progesterone hormone causes the endometrium to thicken. If the egg is not fertilized, the corpus luteum degenerates, levels of estrogen and progesterone decrease, and a new menstrual cycle begins. In regard to PMS, as many as 80% of regularly ovulating women experience some degree of physical and psychological symptomology of PMS during this time.
Symptoms
There are two areas of symptoms when it comes to PMS – psychological and physical. Common psychological symptoms include depressed mood, anxiety, mood swings, irritability, decreased interest in regular activities, difficulty concentrating, fatigue, change in appetite, sleep disturbances, and feeling overwhelmed. Common physical symptoms include breast swelling and tenderness, bloating, weight gain, edema, acne, and headaches. Not every woman will have all of these symptoms, and symptoms will vary from person to person.
Diagnosis
Simply put, to be diagnosed with PMS both physical and psychological symptomology should be present during the luteal phase of the menstrual cycle (about seven to fourteen days before menses). The symptoms are associated with clinically significant distress or interference with work, school, and usual social activities. These symptoms will not be an exacerbation of another disorder such as depression, panic disorder, or other physical disorders.
Usually the criterion for PMS is confirmed by prospective daily ratings of two symptomatic cycles, followed by the resolution of symptoms after the onset of menses. A gynecologist or primary care physician may give you a paper to fill out or you keep a journal of your symptoms for diagnostic purposes.
Treatment
Even if you have not been diagnosed, many women know they are going through PMS and use alternative therapies, nutrition, and physical exercise to help alleviate their symptoms. Women with diagnosed PMS can use conventional medical therapies. We will go through all of these types of treatment, but always talk with your primary care physician or gynecologist before undergoing any type of treatment.
Conventional Medicine
Conventional medicine requires diagnosis and prescriptions from a medical doctor, physician assistant, or licensed nurse practitioner. For bloating symptoms, a mild diuretic can be prescribed or an over-the-counter brand can be recommended. For mild anxiety an anti-anxiety medication may be used. For depression, some SSRIs are prescribed, but are usually reserved for severe cases.
One preparation has been affective in at least one randomized, controlled trial and that includes the following:
- 1200 mg calcium carbonate – mood and behavior control
- 100 mg spironolactone – mood and bloating
- 25 mg buspirone – premenstrual anxiety
Some studies also show that continuous use or 24 out of 28 day use of an oral contraceptive containing the progestin drospirenone can be beneficial.
Alternative Medicine
According to BMC Complementary Alternative Medicine, acupuncture and herbal medicine has been a recent favorable therapeutic approach to relieve PMS symptoms. Thus, they aimed to review the affects of the treatment path. The review included randomized controlled clinical trials from 2002 to 2012, which yielded nineteen studies. Different acupuncture techniques and herbal prescriptions were evaluated for the treatment of PMS.
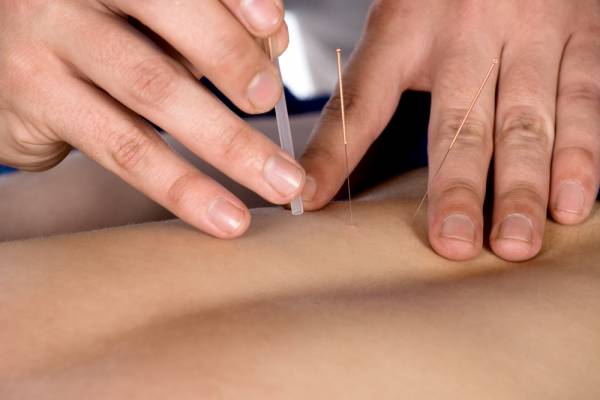
Acupuncture and herbal prescriptions showed a fifty percent or better reduction of symptoms compared to initial states. In both treatments, no serious adverse affects were reported, which made this treatment option favorable to many sufferers. Unfortunately, limited evidence supports the efficacy of alternative medicinal interventions for PMS.
Diet
As with daily life, usually if you eat like crap, you feel like crap. Same words apply with PMS. Here are things to watch for:
Too much sugar and refined foods: Dr. Abraham showed a link between sugar and PMS when he discovered that women with PMS consumed about 275% more refined sugar than those without PMS. Think ladies, how much sugar do you eat when you are PMSing? This massive intake can wreak havoc on your body. This may be one of the reasons why women experience symptoms of hypoglycemia after eating (i.e. mood swings, anxiety, irritability, and headaches). So, ladies, cut the sugar and starchy food out of your diet, especially while you have PMS.
Too much salt: Slow down on your salt intake if you are a heavy salter or salty food lover. It can exacerbate symptoms of water retention and bloating.
Too much caffeine: Too much coffee, tea, or energy drinks (specifically), can cause an increase in anxiety, irritability, agitation, breast tenderness, poor sleep, and depression. Caffeine and other methylxanthines can activate stress hormones and encourage fluid retention.
Vitamins: Specific vitamins can help with PMS symptoms. Try to get as much as you can from your food intake, but if you take supplements, then remember it’s important to take your vitamins with food. Each vitamin listed helps with the following symptoms:
-
Vitamin E: Breast tenderness, anxiety, fatigue, depression, and insomnia
-
Vitamin B6: Hormone balance, mood regulation, and PMS acne
-
Magnesium: Stress, anxiety, water retention, fatigue, pain, breast tenderness, weight gain, and hormone balance
-
Zinc: Hormone balance
-
Chromium: Blood sugar balance, sugar cravings, mood swings, irritability, and headaches
Exercise
If you already exercise, there is no reason to stop when you feel PMS symptoms. If you need a reason to exercise and you have serious symptoms of PMS, this may get you to start. Studies show that women who exercise regularly have PMS less frequently than women who lead sedentary lifestyles.
Studies also show that women who regularly exercise reported fewer PMS symptoms and suffer less from mood swings, poor concentration, depression, anxiety, and pain. Exercise raises endorphins and serotonin boosting mood and reducing pain and inflammation. Exercise also helps burn fat for a healthy BMI (a higher level of obesity means a higher level of PMS symptoms).

PMS may be part of your regular luteal phase, but there are ways to combat your symptoms. If you suffer from severe PMS, consult your primary care physician or gynecologist because it could mean you are suffering from another disorder called PMDD (premenstural dysphoric disorder). These treatment options outlined above can help make your life easier for the seven to fourteen days you have PMS, but always consult your primary care physician before starting any treatment option.
References:
1. Hacker, NF. et. al. Hacker and Moore’s Essentials of Obstetrics and Gynecology (Philadelphia: Elsevier, Inc, 2010), Kindle Edition
2. Reid, RA and Weber, AA. Women’s Health, The Clinical Medicine Series(Washington: Amazon, 2014), Kindle Edition
3. Perry, S. Premenstrual Syndrome, The Essential Guide (Great Britain: Need2Know, 2012), Kindle Edition
4. Tate, P. Seely’s Principles of Anatomy and Physiology (New York: McGraw Hill Companies, 2012), 782-795
5. Sayehimiri K, et. al. “Epidemiology of Premenstrual Syndrome (PMS) – A Systematic Review and Meta-Analysis Study.” Journal of Clinical Diagnostic Research (2014): 106-109, accessed April 13, 2014. DOI 10.7860/JCDR/2014.8024.4021
6. Jang, Su Hee. et. al. “Effects and Treatment Methods of Acupuncture and Herbal Medicine for Premenstrual Syndrome/Premenstrual Dysphoric Disorder: Systematic Review.” BMC Complementary and Alternative Medicine (2014): 14:11, accessed April 13, 2014. DOI 10.1186/1472-6882-14-11
7. Verma, RK et. al. “Review on Treatment of Premenstrual Syndrome: From Conventional to Alternative Approach.” Journal of Basic and Clinical Physiology and Pharmacology (2014): ePub first, accessed April 14, 2014. DOI 10.1515/jbcpp-2013-0072.
Photos courtesy of Shutterstock.






