When we use imaging to look at the spine, we can see things like degeneration, disc bulge, scoliosis, or maybe even an extra vertebra. These findings can make clients feel like they are broken or something is wrong with them. They will probably also assume the findings on this MRI are the reason or root cause for their pain.
I explained previously that just because an X-ray, CT scan, or MRI shows an “abnormality” does not necessarily mean someone needs fixing. Often, that abnormality is simply that person’s normal.
An awareness is starting to trickle down to clients and the general public that an abnormal diagnostic image is not necessarily relevant to treatment. But for some reason, this logic seems to be isolated to the spine. An abnormal result in any other body part still seems to lead everyone to believe that it is also the reason for pain, injury, or dysfunction.
If people can have abnormal results in the spine but are otherwise completely asymptomatic, why can’t the same be true for other parts of the body, like the hip or the shoulder?
Diagnostic imaging can show abnormalities (like this rotator cuff tear), but those don’t always translate to dysfunction.
Who Has “Normal” Shoulders?
This question was the subject of a study published in the American Journal of Roentgenology. Researchers analyzed findings of shoulder ultrasounds to determine the prevalence of any “abnormality” in otherwise healthy, asymptomatic men. The study looked at 51 men ages 40–70 who had no symptoms in either shoulder.
An ultrasound of one shoulder per patient was performed by a sonographer according to a defined protocol, which included imaging of five areas:
- Rotator cuff
- Tendon of the long head of the biceps brachii muscle
- Subacromial-subdeltoid bursa
- Acromioclavicular joint
- Posterior labrum
The scans were then analyzed by three radiologists in consensus, with subtle or questionable findings (mid tendinosis, bursal prominence, and mild osteoarthritis) being omitted.
When Problems Aren’t a Problem
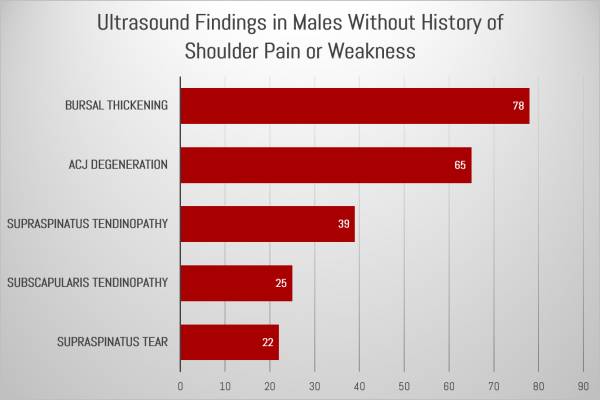
Researchers discovered subacromial-subdeltoid bursal thickening in 78 percent of the subjects. Bursa are thin, fluid-filled sacs that reduce friction in joints and help facilitate gliding of muscles and tendons over and through them. Typically, thickening of the bursa indicates inflammation and has been thought to cause pain.
But the men in the study were completely asymptomatic.
Further analysis showed the following:
- Acromioclavicular joint osteoarthritis in 65 percent of the men.
- Supraspinatus tendinosis (damage/degeneration of a tendon of one of the rotator cuff muscles) in 39 percent of the men.
- Subscapularis tendinosis (another rotator cuff muscle) in 25 percent of the men.
- Partial-thickness tear of the supraspinatus tendon (a third rotator cuff muscle) in 22 percent of the men.
- Posterior glenoid labral abnormality (an abnormality in the fibrocartilage ring that runs around where the upper arm bone fits) in 14 percent of the men.
All of these men had abnormal anatomy revealed in their ultrasound, but were asymptomatic. So are they really abnormal?
In Plain English, Please
To translate all the anatomy-nerd-speak, the study found that abnormalities were found in 96 percent of men who have absolutely no pain or issues with their shoulders. They are simply living their lives as usual, but an ultrasound shows an “abnormality.”
Just like we learned with MRI for the spine, results of ultrasounds for shoulders should be interpreted closely and combined only with clinical findings to determine the cause of symptoms. Seeing a skilled physical therapist who can assess the reason for shoulder pain is still required, regardless of what an ultrasound finds. Maybe you are one of the individuals who has a tear in your shoulder, but it is causing you no pain. If this is the case, imagine how upset you would be if you repaired the tear, only to find out that your pain came back because the root cause of your injury was never discovered or rehabilitated?
If It Ain’t Broke…
Always read results of imaging with an understanding that they do not mean you are broken. Imaging is a fantastic tool, and at times is incredibly important for injuries. As a physical therapist, there have been times when I have had to push for images to confirm clinical diagnosis. But the imaging results cannot be viewed in isolation from the bigger picture.
Just because the results of an X-ray, MRI, or ultrasound show something abnormal, please don’t take that as a reason to stop working on your strength, mobility, or range of motion. You are not “broken” or “abnormal.” Stay the course, keep working hard to rehabilitate your injury, and recognize the results for what they are: a single piece of the overall you.
More Training and Rehabilitation Science:
- You Are Not Normal – Here’s Why
- Myths About Disc Bulges: They Are Not Forever – But Training Is
- Get the Diagnosis Right: It’s Not Tendonitis, It’s Tendinosis
- New on Breaking Muscle Today
Image courtesy of Wikimedia Commons.






